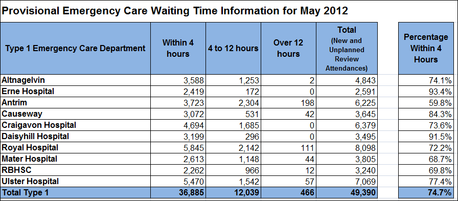
- In Type 1 emergency care departments, the percentage of patients attending that were either treated and discharged home or admitted within 4 hours decreased by 5.3 percentage points, from 71.6% to 66.3% ).
- In Type 2 emergency care departments, the percentage of patients attending that were either treated and discharged home or admitted within 4 hours decreased by 4.6 percentage points, from 87.5% to 82.9% .
- In Type 3 emergency care departments, the percentage of patients attending that were either treated and discharged home or admitted within 4 hours remained at 100.0%.
- The number of patients that waited longer than 12 hours to be either treated and discharged home, or admitted, increased slightly (34, 3.4%) from 987 to 1,021. In particular, performance declined notably at the Ulster between January and March, from 223 to 397.
|
Between March 2012 and March 2013:
0 Comments
A group of senior consultants in Antrim Area Hospital have described the A&E department as "ineffective and unsafe".
The claim was made in a letter from seven consultants in the department to the hospital's medical director. http://www.bbc.co.uk/news/uk-northern-ireland-22157566 Views of NHS changes from mainland UK - http://www.hospitaldr.co.uk/blogs/our-news/review-on-future-of-urgent-and-emergency-care-launched
A major review of urgent and emergency services has been launched by the NHS Commissioning Board to establish proposals for the best way to organise care in England. The review, led by Medical Director Sir Bruce Keogh, will work with clinical commissioning groups (CCGs) to develop a national framework offer to help them ensure high-quality, consistent standards of care across the country. Sir Bruce said: “The NHS is there for all of us and should offer appropriate, effective and rapid care whenever and wherever it is needed. “Treatments for many common conditions such as heart attacks and strokes have evolved considerably over the last decade and are now best treated in specialist centres. Yet we know people want their A&E nearby. “This makes me think we need to review the increasingly complex and fragmented system of urgent and emergency care, so that sick, anxious and often frightened people can get what they need when they need it.” The review comes as a number of hospital A&E departments are under threat of closure, provoking public outrage. The NHS Commissioning Board stresses that local commissioning will be at the heart of this review, which follows the Board’s commitment in its recent planning guidance. It aims to enable CCGs to shape services for the future and put in place arrangements that meet the needs of patients. It plans to publish emerging principles for consultation in the Spring. In its planning guidance, published late last year, the NHS Commissioning Board said it would review urgent and emergency care as part of plans for more seven-day services. As well as seven-day working, the review aims to help CCGs find the right balance between providing excellent clinical care in serious complex emergencies and maintaining or improving local access to services for less serious problems. It will set out the different levels and definitions of emergency care. These range from top-level trauma centres at major hospitals to local accident and emergency departments and facilities providing access to expert nurses and GPs for the treatment of more routine but urgent health problems. As well as looking at how emergency care is provided, the review will also assess transfer processes between these levels of emergency care. The NHS Commissioning Board also says it wants to improve public understanding of the best place to go for care. By helping the public to go to the right place first, both they - and those who have very serious illnesses and injuries - will be seen more quickly by specialist clinical teams with the right qualifications and facilities. It stresses that the pattern of urgent and emergency care, including the number and location of services, will continue to be de developed locally to meet the different needs of urban and rural communities. The review aims to provide a national framework so high quality, consistent standards are offered across the country. In future, planning reconfigurations should take account of the review’s conclusions, the emerging evidence and the national framework. The Foundation Trust Network recently published a briefing document summarising the results of their A&E 2012 benchmarking study. It found that the majority of trusts are losing money on their A&E services. It called on the Department of Health to re-examine the policy of paying for some emergency admissions at 30% of the standard tariff, and called on the risks and responsibility for avoiding emergency admissions should be more fairly shared between acute trusts and primary and community care. It also found that trusts with primary care or urgent care centres within their A&E departments have faster average treatment times. And trusts that use senior clinicians as part of a rapid assessment team have faster initial assessments for the most acute A&E patients Nearly half of all A&E attendances for older patients (75yrs+) end in admission. Multidisciplinary teams in A&E reduce admissions of elderly patients, and trusts have reduced reattendance rates by providing comprehensive information and follow up advice. Dr Clive Peedell, a clinical oncologist and co-leader of the National Health Action Party, said A&E closure was often the “death knell” for a hospital. He said: “Once you lose A&E, you lose all your acute admissions. It’s like dominoes. It’s a way to close a hospital. There seems to be a drive to close hospitals on an ad hoc and financially-driven basis. There’s a definite agenda to treat more people in the community - but the capacity isn’t there. “We welcome the review but it needs to be open to debate. It should not be a central diktat.” Valerie Jackson has now been removed from the Board of the Northern Health & Social Care Trust. Although this removal is welcomed by Save The Mid, other people involved in the detriment of acute care within the Northern trust should also be removed from managerial positions, namely Dr Oliva Dornan. Save The Mid will find it hard to believe that Valarie Jackson rarely made a medical decision without first consulting Dr Oliva Dornan first.
Save The Mid has constantly questioned the creditability of the decisions made bu the Directors of the NHSCT, the decisions that were made in the name of patient safety have led to some of the worst episodes of patient safety within the trust. A further review should be under taken by the DHSSPS and Heath Minister to investigate past decision made by Valerie Jackson. The director was involved in the controversial decision to remove acute services from the Mid Ulster hospital, the closure at the time was classed a crisis closure. What needs to be answered who caused the crisis closure ? Save The Mid will keep constant pressure upon the board of the NHSCT with the view that Chairman Jim Stewart be brought to Health Minister Edwin Poot's and questioned on the activity of the NHSCT board during his rein as chairman. Valerie Jackson took up the post of Director of Acute Hospital Services on 2 November 2009. She trained as an RGN in the Royal Victoria Hospital (1985-1988) gaining her midwifery qualification in 1991. Having held many nursing posts in a wide range of hospital and community settings, she joined the Northern Ireland General Management Training Scheme in 1995 which involved working in range of posts in a variety of Trusts in Northern Ireland. She was appointed Project Manager for Phase 1 of the Royal Belfast Hospital for Sick Children in 1997. Between 1998 and 2003 Valerie worked as Directorate Manager for Medicine, General Manager for Emergency Care and Divisional Manager for the Division of Medicine and Surgery before leaving the Royal Victoria Hospital in 2003 to take up post as Director of Nursing and Primary Care in the Ulster Community and Hospitals Trust. In 2007 she was appointed to the position as Director of Older People Medicine and Surgery in the Belfast Trust and was also Executive Director for Nursing until June 2009 when she stood down from that role to allow Trauma and Orthopaedic services to join the Older People Medicine and Surgery Service Group. Reponsibilities
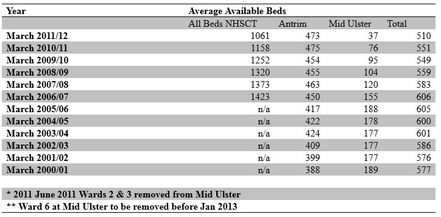 Northern Trust cut Mid Ulster Hospital lifesaving operations Inpatients within the Mid Ulster Hospital faced the largest cuts in hospital beds in the entire Northern Health & Social Care Trust (NHSCT) during 2011/12. This is scandalous considering the bed crisis within the Trust which led to Valarie Jackson, head of acute services NHSCT, stating in response to the Rutter and Hinds report that 90% of all waits in A&E are because there are no beds. Currently there is an average of 37 inpatient beds at the Mid Ulster Hospital, this is a fraction of the former 189 fully acute inpatient beds it had 10 years ago, at the moment Thompson House is to close by Jan 2013, and these patients are to be moved to ward 2 within the hospital. As of yet this relatively new ward cannot be used as there is a problem with the floor. This beggar’s beliefs as these problems were not occurring when the ward was in use just over 1 year ago, if these issues were present while the ward was operational then serious questions must be raised about the Northern Trusts ability to act on clinical risks properly. Within the Northern Trust for the year 2011/12 a total of 97 beds was lost, 38% of which were in the Mid Ulster hospital. Since the Northern Trust came into effect a total of 362 beds have been lost. Although the Trust intends to open a new 24 bedded ward at the Antrim there will still be a net loss of beds, bed shortages are one of the most clinical dangers within the Trust, one which they compound by their own actions. Does it make any sense that the Trust cut more beds? There has to be some accountability to this move and every step must be taken to insert more inpatient beds to the Mid Ulster Hospital for patients that do not require 24 hour consultant oversight, like it was intended to have. The availability of inpatient beds affects the Mid Ulsters hospitals abilty to perform remaining services in day case surgery and inpatinet care. Currently within the hospital in terms of inpatients the following services can be facilitated; General Surgery, ENT, Ophthalmology, Pain Management, General Medicine, Gastroenterology, Haematology (Clinical), Neurology, Paediatrics, Geriatric Medicine, Gynaecology, General Practice (Other). If bed losses are continued then these services will not be sustained, so in essence the Northern Trust are creating an environment in where by their own actions they are fracturing these services so that in the future they can remove them. This tactic was used to close maternity and the A&E, they got away with it then and without opposition they will get away with it again The Population plans produced by the Dept Health specifically state for Mid Ulster Hospital to lose more services and turn the Hospital into a health center, the plans state; “There is a need to rationalise the delivery of day surgery services currently provided from Whiteabbey and Mid Ulster Hospitals to ensure we make best use of skilled surgeons, doing more of this work within Antrim and Causeway acute sites. Whiteabbey and Mid Ulster, along with the other community hospitals have an important role to play in developing more local provision particularly in relation to community/primary care led services. This will be one of the areas we will explore within the Integrated Care Partnerships as they develop, aiming to strengthen the working arrangements that are already in place between the Trust and local GPs.” The Northern Trust has seen excessive waiting times and lack of internal capacity in Inpatients, this has led to patients being sent to the independent sector for treatment at a further cost to the public. As at the 31st July 2012 there were 1,179 patients waiting over 13 week for their day case or inpatient surgery within the Trust. A further 429 patients were waiting in the Independent Sector for treatment. There is a proven lack of capacity within the Trust to meeting an ever increasing demand for services. For the year 2011/12 the Northern Trust held 29,734 sessions within its operating theaters 4,517 of which were held in the Mid Ulster Hospital. Already in the space of a year despite an increasing demand for service the Northern Trust have carried out 1,361 less non-elective inpatient cases within the Trust, with Mid Ulster Hospital there were over 2 thirds (68% drop, 695 actual) less life saving cases held in the hospital;
Two General Medicine wards in Mid Ulster Hospital closed in June 2011. Activity in Mid Ulster Hospital increased due to the specialty of some beds changing from a General Medicine specialty to a Geriatric Medicine specialty. Services at the Mid Ulster hospital are continuously under treat and are being removed by stealth, it is about time all those in a position to prevent this rot speak out for Mid Ulster Patients and for a Hospital that has given birth and saved the lives of so many Mid Ulster residents. Reference: Elective: In medicine, something chosen (elected). An elective procedure is one that is chosen (elected) by the patient or physician that is advantageous to the patient but is not urgent. Non – Elective: Emergency surgery is non-elective surgery performed when the patient's life or well-being is in direct jeopardy. Largely performed by surgeons specializing in emergency medicine, this surgery can be conducted for many reasons but occurs most often in urgent or critical cases in response to trauma, cardiac events, poison episodes, brain injuries, and paediatric medicine. Save The Mid are appalled that the Northern Health & Social Care Trust (NSHCT) has topped the list of shame for the longest time in being taken into A&E until admission to the Hospital. What is more frightening is that the longest wait as released by the Daily Mail as 50:33 may not be fully accurate as time spent by a patient in the short stay ward or clinical decision area is not counted as time spent waiting.
http://www.dailymail.co.uk/health/article-2204872/The-NHS-Trusts-leaving-patients-trolleys-50-hours-How-did-YOUR-hospital-perform.html Save The Mid already submitted a patient survey to government concerning the treatment of patients from Magerafelt and Cookstown in Antrim A&E, this survey went unheard or acted on - https://docs.google.com/file/d/0B3yFZ5whLJ8zMjQ0NDhmZmQtOGQ1Yy00NDQ4LWIxODEtNmI2M2MzZjE2ZDU2/edit?pli=1 Save The Mid have also alerted RQIA on the ‘Corridor ward’ that is now in place at Antrim to line patients up as there is no room - http://savethemid.weebly.com/1/post/2012/09/antrim-area-hospital-corridor-ae-ward-out-of-sight-out-of-mind.html For 2 years Save The Mid have been repeatedly asking government to reinstate Acute services to Mid Ulster as the are required in Mid Ulster for Mid Ulster residents but also to make safe other service in areas such as Antrim and Coleraine. Mid Ulster Hospital over the past 6 years has faced cuts in acute and inpatient care, the NHSCT were pre warned in a risk assessment in 2006 that network hospitals could not sustain it service if the shut down the Mid Ulster Hospital. This is exactly what the NHSCT did and is a direct reason as to why the appalling conditions seen in Antrim Area Hospital. Patients are suffering as the NHSCT made a clinically unsafe decision. Recently a report commissioned by Health Minister Edwin Poots, carried out by Rutter & Hinds highlights some of the issues in the Hospital, it was later stated by Valarie Jackson (Exe Acute services NHSCT) that 90% of those waiting for admission was because there was no bed to admit them to, yet the NHSCT continue to cut beds year on year. It is quite simple capacity is full at Antrim, it was full before they shut the mid Ulster Hospital of acute services and now with a further loss of Thompson House more pressure will be put upon Antrim Area Hospital. The question that must be answered now is when Edwin Poots stated on Hansard it was a mistake to shut services at Mid Ulster, will he now fix this mistake. Save The Mid will be represented in a series of public debates surrounding health in Mid Ulster, this scam that we are getting better services must end and accountability brought into effect. 3 of the worst affected hospital for waiting are in N Ireland, either Trust Chiefs and the Minister step up or they should do the right thing and step down. Hugh McCloy Save The Mid 07871503189 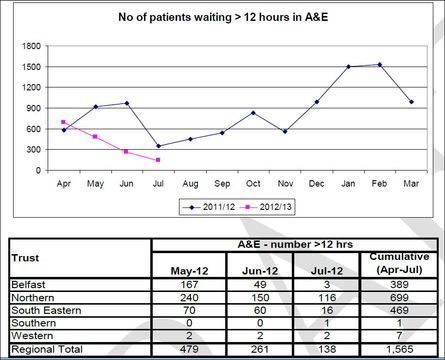 HSCB Trust Performance Four out of five Trusts have improved their performance since June and the fifth has maintained its position. The Board and PHA are continuing to take forward a programme of work with all Trusts to bring about a step change in A&E performance. There has been a significant month on month improvement in performance for this standard with particularly large reductions in breaches within Belfast Trust. The majority of the breaches in July are within Northern Trust also these are reduced from June 2012. It should also be noted that Northern Trust was the only Trust to have an increase in A&E attendances between June and July 2012 (from 9503 to 9799 attendances). The Board (HSCB) and PHA are continuing to take forward a programme HSCB of work with all Trusts to bring about a step change in A&E performance and the Northern Trust position will be addressed as part of this process. A&E performance in May 2012 shows that not one A&E in Northern Ireland met the Ministerial target of 95% of patients to be seen within 4 hours.
The worst offender is the ever probmatic Antrim Area Hospital, not only did it have the most patients waiting over 12 hours to been seen only 59.8% of patients were seen in under 4 hours. Recently the NHSCT have released to local papers across the Trust that the new A&E will benefit people in local communities, what local communities are looking to know is what are the Turst do to benefit people now. There has been a scary silence on the political front, when taking into account 466 patients waited over 12, this is the equivalent of waiting at least 233 Days being spent waiting in A&E's across Northern Ireland in May 2012*. *this figure does not take into account patients waiting 4-8 or 0-4 hours http://www.dhsspsni.gov.uk/index/stats_research/hospital-stats.htm There have been several reactions to the new A&E unit at Antrim Area Hospital:
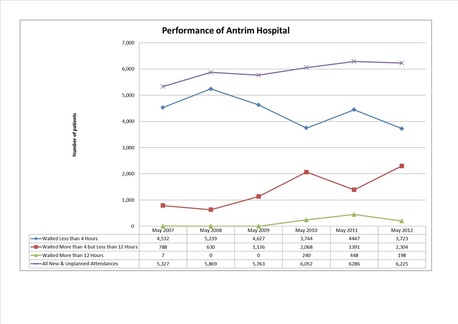
Several questions must be answered before further reconfiguration of services: will the new A&E that is the same operational size as the previous one in Antrim really be able to serve 90,000 patients a year, & will it be able to admit patients any faster than its predecessor. In May 2012 the performance of Antirm A&E was the third worst in its history, yet there has been silence by the Health Minster and politicians regarding this. The below graphs show the constant downward spiral of performance at the troubled Antrim Area Hospital. 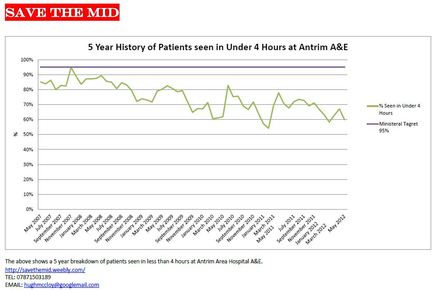 Graph to show 5 year performance of Antrim A&E. Green line is performance, Purple line is the target it should be at. 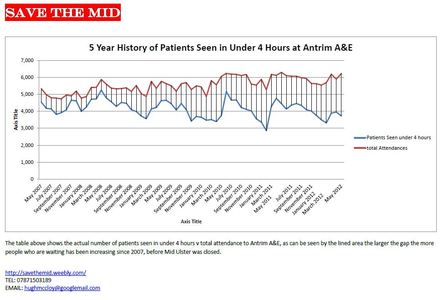 Graph to show the amount of patient treated between 4-12 hours at Antrim Area A&E. The bigger the lined area the more patients waiting over the target of 4 hours to get treated. ‘Record number’ using ‘Mid’ - claim
Published on Thursday 28 June 2012 11:08 Mid Ulster Mail A RECORD number of people are attending the Mid-Ulster Hospital’s Minor Injury Unit as Antrim Area Hospital’s waiting times continue to suffer, according to a local health group. Last month the Minor Injury Unit (MUI) at the Mid-Ulster Hospital recorded its highest number of attendants to date. Over 730 people passed through the doors of the 9am to 5pm unit, which replaced the Magherafelt hospital’s emergency department in May 2010. Pressure group ‘Save the Mid’, who recently submitted details of a patient survey of Mid-Ulster residents to the Health Committee, said it is now time for the Northern Health and Social Care Trust (NHSCT) to begin utilising more acute services back into the Hospital Road site. Read Full Article Here: http://www.midulstermail.co.uk/news/local/record-number-using-mid-claim-1-3998006 |
Media/Reporters - Please Read
You are welcome to use our material, whether it’s the story itself or the graphics. We do want to share our stories with as wide an audience as is possible but we ask that you respect our three simple conditions. 1. You alert us to your plans to publish. 2.That you credit “Save The Mid” in any broadcast or publication of a story that we have originated. If you are a newspaper, the credit should come in one of the first three paragraphs. 3. If publishing online, that you link back to us. Archives
January 2018
Categories
All
|

 RSS Feed
RSS Feed
