The poll also shows that 48% of family doctors think that patients now have to wait longer for a GP appointment, while four in five GPs are more likely to want to quit the profession than they were five years ago.
The fieldwork for the survey was conducted between 5-11 June 2013 by Research Now on behalf of the RCGP. Researchers reported on a random sample of 258 GPs across the UK; 210 from England; 25 from Scotland; 14 from Wales; and 9 from Northern Ireland
The poll also revealed that:
- 55% of GPs conduct 40-60 patient consultations each day
- 46% of GPs work at least 11 hours each day in surgery
- 84% say their workload has increased substantially
- 58% of GPs work at least until 7pm
The survey comes after GP's threatened to revolt over proposed changes through Transforming Your Care unless the GP contracts were changed in March 2013.
However GP's reached a deal with Health Minsiter Edwin Poots in April 2013 in exchange for work concessions through the Quality & Outcomes Framework, which is a system for the performance, management and payment of GP services. 2011/12 QOF report N Ireland.
“The results of this poll show that general practice is in a state of crisis and that urgent action must be taken to restore the ability of our family doctors to deliver safe patient care for all.
“General practice is at the heart of the National Health Service, and if it starts to buckle, the whole of the health service starts to buckle and patient care in both primary and secondary care will suffer.
She added: “General practice has radically altered over the last five years, with ballooning workloads, and more and more patient consultations having to be crammed into an ever expanding working day – as the patient population grows older and increasingly suffers from an increasing range of ailments.
“The overwhelming pressure that many GPs now feel is leading to an upsurge in work-related stress and other health issues and we need to ensure that we can deliver safe care for all our patients. General practice must be given at least 10% of the ring-fenced NHS budget.”
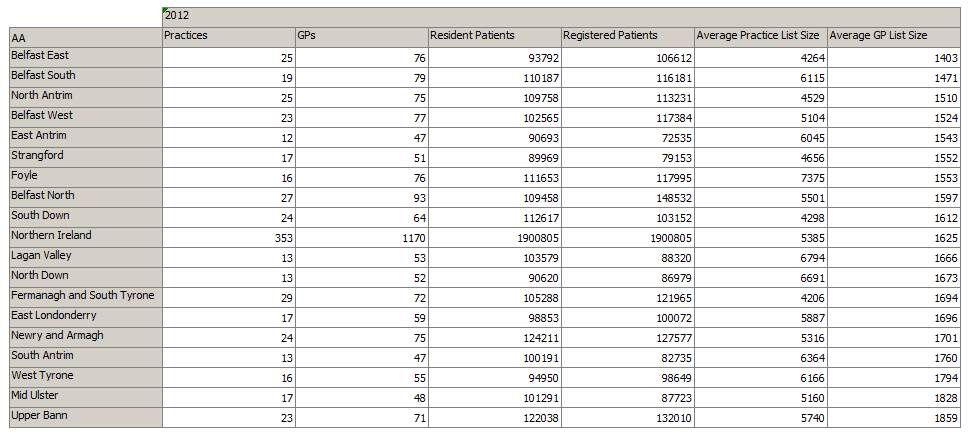
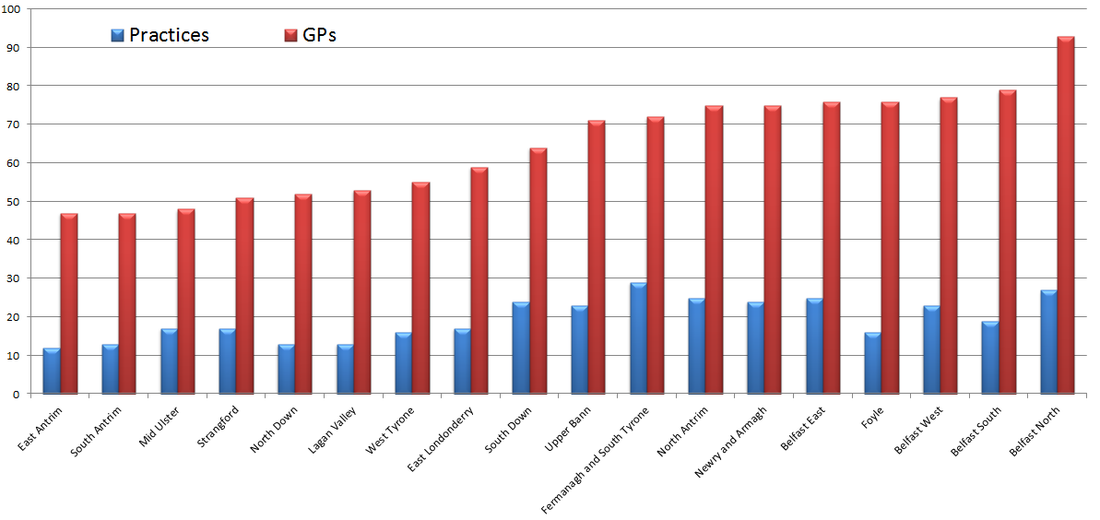
Upper Bann & Mid Ulster Have Largest GP List Sizes In Northern Ireland
The minor injury unit that is left behind in its place is only open 9am-5pm excluding weekends and bank holidays, with an out of hours service that is restrictive in its use.
We are not facing a Transformation Of Care in Mid Ulster, we are facing the Termination of Care in Mid Ulster.
Universal Out Of Hours Health Care Number
The NHS 111 number has be highly criticized by the medical profession for not being GP led, The 111 line is being phased in by the Government to replace the old NHS Direct service, but unlike its predecessor it is staffed mainly by call center workers with little nursing training.
NHS 111 Rejected By BMA in Northern Ireland
GPs at the conference also expressed a desire to take back control of the out-of-hours GP services in the country, and voted in favour of asking the BMA Northern Ireland GPs committee to lead on the issue.
Could These Changes Led To Increased A&E Attendances & Greater Reliance On The Private Health Sector
"There are several factors that have fueled the Health Care Crisis that we face in Northern Ireland Today: massive health cuts by successive health ministers and governments since the establishment of Stormont in 1998 that led to hospital and bed closures leaving patients today stuck in A&E wards unable to go elsewhere; an Out Of Hours services that is inadequate, run by the private sector for profit and does not have the staff or resources to act as a stand alone unit; the almost complete closure of government residential care homes fro children, mental health patients and the elderly; a lack of community care services that had led to bed blocking; a reliance of Trusts to use the private sector has been building for over 10 years, a reliance that stops Trusts from developing their public services despite the cost." Hugh McCloy - Save The Midm

 RSS Feed
RSS Feed
