THE Northern Trust has placed a restriction on visiting at Antrim Area Hospital following an increased incidence of vomiting and diarrhoea. So
|
AMBULANCES were diverted from the Causeway Hospital in Coleraine for several hours on Monday night, because of an increased pressure at the accident and emergency unit. Link
Western Trust has closed Ward 3 at Altnagelvin to admissions and asks public not to visit patients if they have been feeling unwell themselves Link THE Northern Trust has placed a restriction on visiting at Antrim Area Hospital following an increased incidence of vomiting and diarrhoea. So
0 Comments
April 2011 - March 12:
April 2012- Jan 2013 (still Feburary and March to be added)
While the Trust have reduced the amount of C DIFF infections it is seeing a high percentage of patient deaths. The NHSCT has seen one of the worst outbreaks of C DIFF in the past ten years in the UK with 31 patients dying during the major outbreak in 2007-2008. The Inquiry Report was published on 21st March 2011. The Inquiry had one finding and made twelve recommendations. The Clostridium Difficile Report is now available and can be accessed by selecting Inquiry Report.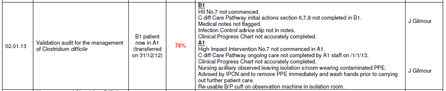  A recent audit of wards A1 and B1 at Antrim Area Hospital shows a low level of compliance against audit targets. The Northern Health & Social Care Trust sent 15, 000 plus patients private in order to deliver the support of achieving Backstop Waiting Times position (references, pages; 38, 39, 40, 41 : link).
Backstops were created in waiting lists by the Trust in conjunction with the Health & Social Care Board, this allowed the trust to over run and miss targets without fear of reprimand. According to most recent data (1st April 2012 4th Jan 2013) the Northern Trust have sent 2,426 Daycase/inpatient to the private sector and 12,889 outpatients to the private sector, in total a 15, 315 patients. The current Ministerial target for daycase/inpatients in that 50% of patients should be treated within 13 weeks and for outpatients 50% of patients should wait no longer than 9 weeks for an appointment. These targets were reduced at the start of the new Assembly term in 2011, previously targets were (reference, pages; 46, 47: NHSCT): ● No patients should be waiting longer than 13 weeks for inpatient or daycase treatment ● No patients should wait longer than 9 weeks for a 1st outpatient appointment These targets have reduced over the years to try and allow for poor performance within the Trust but even with this drop in the Trust are failing. According to the performance report 1,446 patients are still waiting over 13 weeks for treatment in daycase/inpatient with a further 3,642 patient still waiting over 9 weeks for the first outpatient appointment. Other areas are also affected by poor performance: ● Diagnostics 1,484 patients are waiting over the 9 week target for cardiac ● Allied Health Professionals 201 patients are waiting over the 9 week target for occupational therapy The question that must be answered is not why are 15,000+ patients being sent into the private sector to beat waiting lists, it is why have services not increased to meet the demand of the population within the NHSCT. The Ulster Hospital recently had to cancel up to 30 operations a day due to lack of capacity, now we see the NHSCT have to make more use of the private sector. This is yet another failure by the NHSCT managers to plan for the future and fully deliver, these extra sessions are specifically to beat waiting lists, waiting lists that only developed due to lack of capacity within the Trust to meet the needs of its residents. This is directly realted tot he clousre of services at the Mid Ulster For the year 2011/12 the Northern Trust spent £116,435,000 (reference, page 41 link) purchasing care from non government bodies, the private sector, while some of this is spent on nursing and residential homes for elderly patients some of this pot is also spent on sending patients to private hospitals. As of yet the Trust have not released how much the contracts for this extra private care is costing the taxpayer. Serious concerns must be raised within the Northern Health & Social Care Trust regarding Outpatient appointments in which the Trust had to cancel, ( reference, page 20 link) for the year 2011/12 the NHSCT cancelled 5,976 out patient appointments as no consultant was available, on top of this consultants themselves cancelled 17,113 appointments. If you have been a patient, visitor or if you are a member of staff at Antrim Hospital can you please fill out this short survey. http://savethemid.weebly.com/antrim-area-hospital---survey.html
Staff, visitors and patients have not been treated with due respect or due care by management within the Northern Health & Social Care Trust, this is your opportunity to have you opinions heard. Results of this survey will be shared with the Heath Minister and the Health Committee. Both of whom are aware of several risks that have occurred in Antrim Hospital. No personal information is gathered and you will not have to give us your name, we just need your experience. We would take this opportunity to thank the nurses and other front-line staff who at this time are working under considerable pressures, pressures that are purely the fault of bad managerial decisions within the Trust. When we are ill and require admission to hospital the very least the management of the Northern Trust can do is ensure that we have beds that are medically safe to be treated in. Also management should ensure that patients are afforded privacy and human dignity and not have patients wheeled into wards to lay on show beds for the general hospital population to see. It is time to send a message to the Northern Trust management that is loud and clear, we are patients but be are also human beings. A Report published today by the Comptroller and Auditor General, Kieran Donnelly, examines audit issues arising in Health and Social Care sector in Northern Ireland in 2011-12. This is the fourth such report on the Health and Social Care sector. The sector spends more than £4.4 billion a year.
Mr Donnelly said “While 2011-12 was a year where the Health and Social Care sector recorded good financial results it was also a period when a range of important measures of health care performance, including Accident and Emergency waiting times, declined. The Department of Health, Social Services and Public Safety has noted some improvements in the early part of the current year. I will examine if this trend has been sustained in 2012-13.” The GOD COMPLEX and the patient….Things you may assume your doctor tells you.. but he may not….even though he is legally bound to! March 2, 2013 by helenhamill
Things you may assume your doctor tells you.. but he may not….even though he is legally bound to! Things you should be able to TRUST your doctor to do… but you can not!. Am writing this, because sadly, we have personally had direct experience of this. and since then we have found large amounts of anecdotal evidence to suggest that this is a common practice! There are ethical doctors and there are arrogant do not question me practitioners! This is a MASSIVELY important issue to me personally…. and i can’t count the amount of my life that i have spent questioning, researching, and sometimes PROVING that Doctors need to realise they are not infallible! I abhor the God-Complex of many healthcare providers, or to give it the more polite and equally superior and condescending medical term…it is “Medical Paternalism”. A lot of medical legal cases depend on “informed consent” of the patient being given. If you are given ONE tablet, you are meant to understand its use, its reason and its potential side effects. There is a PIL – a Patient Information Leaflet with your drug. This legally warns you of the potential complications….although its only fair to tell you, that through bad experience, we have learned that the PIL in UK may not have the level of detail on complications as the PIL in USA -a more legislative society, seems to merit more ass covering on drug company behalf. If you have any problem then with your medication, as cited on the leaflet, and as firstly explained by the Doctor, then you go back and report it…your Adverse Drug Reaction…and you together discuss new plans of treatment appropriate for your case. BUT in your timed 10 minute slot, is your doctor/GP meant to examine, diagnose, notate and record in your file and explain to you possible problems with meds? YES this stands equally true for: · an adult · a child · a child with mental impairment · an adult with mental impairment so YOU the patient, YOU the parent or YOU the carer should ALWAYS be giving informed consent to any change in prescription or treatment. The GMC is the General Medical Council…the governing body for GPs, specialists, Trust employees….states in its good practice guide some VERY conflicting and contradictory advice! These are available on line at http://www.gmc-uk.org/ where the catchy slogan is “Regulating Doctors, Ensuring good medical practice” Let me give you a few examples, which MAY surprise you. In the GMC “Ethical Guidelines” , in a section called Discussing Side Effects and other Risks: 28. …”the amount of information about risk that you should share with patients will depend on the individual patient and what they want or need to know” 29. .. “you MUST identify the adverse outcomes that may result from the proposed options” now does this mean a doctor, any Doctor decides what I NEED TO KNOW? If he is treating my child, he decides how much information I NEED TO KNOW? i don’t think so!. To compound the confusion i would like to share with you a section from the guidelines given by the Royal College of Paediatrics and Child Health. http://www.rcpch.ac.uk/child-health Many drugs used in children, are not actually licensed for use on children – as they are generally not the trial sample. So doctors make their decisions on use cautiously, i presume, as the effects of these drugs on children are unknown/unrecorded officially. if you google “the use of unlicensed medicines or licensed medicines for unlicensed applications in paediatric practice” you will find the full leaflet, but let me save you time a quote a few bits..they are told “In general, it is not necessary to take additional steps, beyond those taken when prescribing unlicensed medicines, to obtain the consent of parents, carers and child patients to prescribe or administer unlicensed medicines or licensed medicines for unlicensed applications” or in real terms, an adult medication can be used on your child, or a medication designed not quite for the condition they are using it on your child for, and you MAY NOT be given any more information than if he were on Calpol. now i do not want to alarm you, but imagine your child cannot communicate? How are you to know if there are serious side effects if you are not told what to look for? This is NOT good enough to me…as a parent. but the final and most important statement which is my rule of thumb, comes from The GMCin its guidelines for “good practice in prescribing and managing medicine and devices” 71…”you MUST give patients (or their parents or carers) sufficient information about the medicines you propose to prescribe to allow them to make an informed decision.” At this stage i was still galled at the “SUFFICIENT” in this sentence but they put it very definitely in the next sentence when they say: 72…”you must ALWAYS answer questions from patients (or their parents or carers) about medicines fully and honestly!” So next time: § You feel rushed by a GP as he looks at the clock, § You feel a bit unwell on a new tablet, § Your GP refuses to give you information you request from him on a medicine § You visit your child in hospital § or Your parent in care, when you lift up the notes ad see the list of drugs…and almost feel you are being sneaky and will get in trouble § QUESTION, QUESTION, QUESTION EVERYTHING! Read all information you get! Question it! Ask are all the drugs you child is on licensed for use in children! Ask about the cocktail of drugs used on your elderly parent! Do not stop until you are happy that you have full information! Check the possible combinations of repeat prescriptions you are on…! but DO NOT ASSUME that you have so far been given a full disclosure of information…. but GET IT! NOBODY will play GOD with my health or the health of any of my family! Hx The above is part of what Save The Mid have lobbied for in order to create extra capacity at Antirm Area Hospital and also give a service to Mid Ulster residents, these were part of a larger response that was submitted for the Transforming Your Care Health review, the full report can be found here link
Bed pressures have existed in the Antrim Area Hospital since before the removal of services at Mid Ulster Hospital. The decision to shut the Mid Ulster Hospital was proved long ago that it was a clinically dangerous move in terms of the ability of network hospital to handle the extra provision; such is the fragility of Antrim A&E being that less than 1 patient extra on average per hour has collapsed the system From January 2012 Antrim Area Hospital has adopted the use of show beds in wards to try and improve performance, day case beds were removed from their wars and placed in the admission wards, Also the practice of show beds in the wards has now become common practice. A show bed is a bed that has no:
When we take cost cutting exercises like the non-recurrent savings of closing wards 2&3 at Mid Ulster creating a full year equivalent saving of £1,100,000 in 2011, only then to be followed by the expenditure of £946,728 to hire out 15 intermediate care beds and medical cover for 15 beds in a private hospital. Wards 2&3 at the Mid Ulster would have been far cheaper to run and also have a greater capacity. Health Minister Edwin Poots is on record on Hansard stating it was a mistake to shut the Mid Ulster Hospital, now recognising the mistake we must find a way to rectify it. This will only be done by re-introducing services to the Mid Ulster Hospital site. The future of acute care in the NHSCT must be built on solid foundations; we cannot simply allow any future plan for acute care to devoid the Mid Ulster area of any. |
Media/Reporters - Please Read
You are welcome to use our material, whether it’s the story itself or the graphics. We do want to share our stories with as wide an audience as is possible but we ask that you respect our three simple conditions. 1. You alert us to your plans to publish. 2.That you credit “Save The Mid” in any broadcast or publication of a story that we have originated. If you are a newspaper, the credit should come in one of the first three paragraphs. 3. If publishing online, that you link back to us. Archives
June 2019
Categories
All
|



 RSS Feed
RSS Feed
